Or how to manage fatigue
We all get tired. We overdo things and feel physically exhausted. It happens to us all. Usually after a night or two of good quality sleep the tiredness goes away and we’re back to our old selves.
But fatigue is different.
It’s an almost overwhelming physical and/or mental tiredness. And it usually takes more than a night’s sleep to resolve. It generally requires multiple strategies, working together, to help you get it under control.
Many people living with a musculoskeletal condition struggle with fatigue. It may be caused by a chronic lack of sleep, your medications, depression, your actual condition (e.g. rheumatoid arthritis, lupus, fibromyalgia) or just the very fact that you live with persistent pain.
Fatigue can make everyday activities difficult, and can get in the way of you doing the things you enjoy. The good news is there are many things you can do to manage fatigue and get on with life.
Exercise and being active. While this may sound like the last thing you should do when you’re feeling fatigued, exercise can actually boost your energy levels, help you sleep better, improve your mood, and it can help you manage your pain. If you’re starting an exercise program, start slowly, listen to your body and seek advice from qualified professionals. Gradually increase the amount and intensity of activity over time.
Take time out for you. Relaxation – both physical and mental – can help you manage your fatigue. I’m not just talking about finishing work and plonking down in front of the TV – though that may be one way you relax and wind down. I’m specifically referring to the deliberate letting go of the tension in your muscles and mind. There are so many ways to relax including deep breathing, visualisation, gardening, progressive muscle relaxation, listening to music, guided imagery, reading a book, taking a warm bubble bath, meditating, going for a walk. Choose whatever works for you. Now set aside a specific time every day to relax – and choose a time when you’re unlikely to be interrupted or distracted. Put it in your calendar – as you would any other important event – and practise, practise, practise. Surprisingly it takes time to become really good at relaxing, but it’s totally worth the effort. By using relaxation techniques, you can reduce stress and anxiety (which can make you feel fatigued), and feel more energised.
Eat a well-balanced diet. A healthy diet gives your body the energy and nutrients it needs to work properly, helps you maintain a healthy weight, protects you against other health conditions and is vital for a healthy immune system. Make sure you drink enough water, and try and limit the amount of caffeine and alcohol you consume.
And take a note out of the Scout’s handbook and ‘be prepared’. Consider making some healthy meals that you can freeze for the days when you’re not feeling so hot. You’ll then have some healthy options you can quickly plate up to ensure you’re eating well without having to use a lot of energy.
Get a good night’s sleep. Good quality sleep makes such a difference when you live with pain and fatigue. It can sometimes be difficult to achieve, but there are many things you can do to sleep well, that will decrease your fatigue and make you feel human again. Check out our blog on painsomnia for more info and tips.
Pace yourself. It’s an easy trap to fall into. On the days you feel great you do as much as possible – you push on and on and overdo it. Other days you avoid doing stuff because fatigue has sapped away all of your energy. By pacing yourself you can do the things you want to do by finding the right balance between rest and activity. Some tips for pacing yourself: plan your day, prioritise your activities (not everything is super important or has to be done immediately), break your jobs into smaller tasks, alternate physical jobs with less active ones, and ask for help if you need it.
Write lists and create habits. When you’re fatigued, remembering what you need at the shops, where you left your keys, if you’ve taken your meds or what your name is, can be a challenge. And when you’re constantly forgetting stuff, it can make you stress and worry about all the things you can’t remember. Meh – it’s a terrible cycle. So write it down. Write down the things you need at the supermarket as soon as you think of it –a notepad on the fridge is a really easy way to do this. Create habits around your everyday tasks – for example always put your keys in a bowl by the door or straight into your bag, put your meds in a pill organiser.
Be kind to yourself. Managing fatigue and developing new ways to pace yourself is a challenge. Like any new behaviour it takes time, effort and lots of practice. So be kind to yourself and be patient. You’ll get there. It may take some time, and there may be some stumbles along the way, but you will become an expert at listening to your body, pacing yourself and managing fatigue.
Talk with your doctor. Sometimes fatigue may be caused by medications you’re taking to manage your musculoskeletal condition. If you think your medications are the issue, talk with your doctor about alternatives that may be available.
Fatigue may also be caused by another health condition – including anaemia (not having enough healthy red blood cells to carry oxygen around your body), diabetes, high blood pressure, fibromyalgia and being overweight. If you’re not having any success getting your fatigue under control, your doctor may suggest looking into other potential causes.
So that’s fatigue…it can be difficult to live with, but there are lots of ways you can learn to manage it.
Tell us how you manage. We’d love to hear your top tips for dealing with fatigue.
FIRST WRITTEN AND PUBLISHED BY LISA BYWATERS IN OCTOBER 2020
Call our Help Line
If you have questions about things like managing your pain, COVID-19, your musculoskeletal condition, treatment options, telehealth, or accessing services be sure to call our nurses. They’re available weekdays between 9am-5pm on 1800 263 265; email (helpline@msk.org.au) or via Messenger.
More to explore
- I’m a “spoonie.” Here’s what I wish more people knew about chronic illness
healthline
A great way to describe what it’s like to have limited energy to family and friends who want to understand. - Fatigue
Better Health Channel - Fatigue and arthritis
Arthritis Society (Canada) - Managing fatigue
Versus Arthritis (UK)










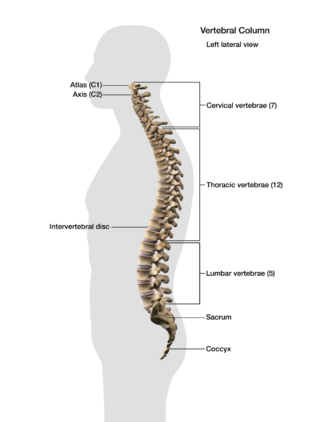 Let’s start with a look at your spine
Let’s start with a look at your spine












